Free Screenings
Join us on Saturdays from 9 am – 2 pm for FREE Screenings
(first come first serve basis, about 8 patient slots available per Saturday)
“This place provides Free Screening every Saturday. I went to check my shoulder problem during their Free Screening event. The physical therapist took enough time to patiently assess me and also explain why I am getting the pain and how to fix it. I went for a few sessions of therapy following that. The treatment and tips they provided were very useful. I am a lot better now and play without limitation. I would recommend you to use their Free screening as they are very good in identifying problems at the very root stage level and treat them too.”
– Bhavya B.
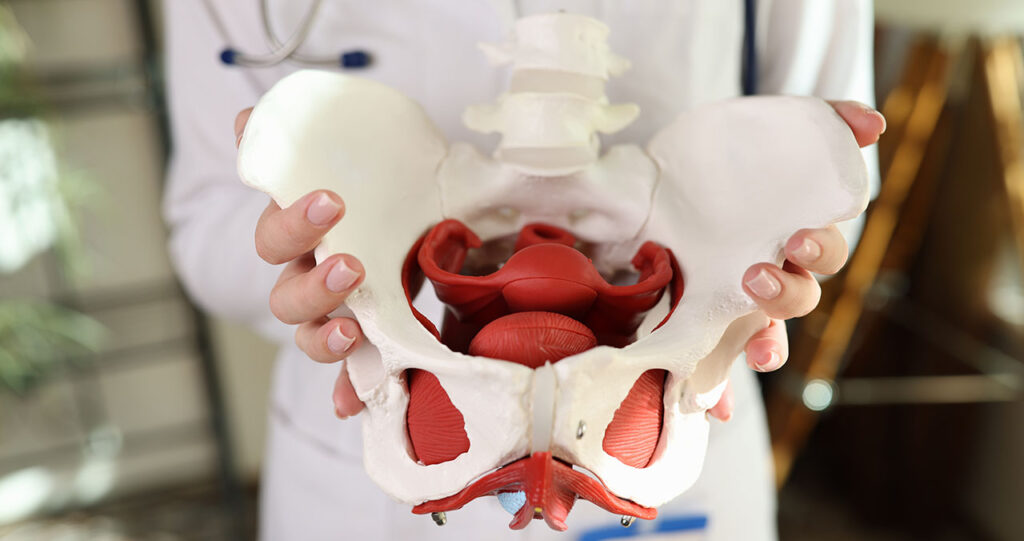
The Relationship Between Lower Back Pain and Pelvic Pain
— March 2025 —

Most of us will experience back pain at some point in our lives. We might get a little too enthusiastic when moving furniture or develop muscular imbalances due to a sedentary job. But sometimes, back pain isn’t really back pain – rather, it’s rooted in dysfunction in your pelvic area.
Unfortunately, pelvic pain is often harder to discuss than back pain. It often stems from dysfunction with your pelvic floor, the band of muscles that support your bladder, bowels, and genitals. It can also indicate an issue with your sacroiliac joints.
Both back and pelvic pain can strike men and women – but women do tend to have more issues with pelvic pain, including pelvic-related back pain. Bodily changes during pregnancy are an especially common culprit.
If you’re dealing with pain in your lower back or pelvic area – or both – call Therapy Fit to schedule an appointment. We’ll help determine the actual source of your pain so you can find lasting relief.
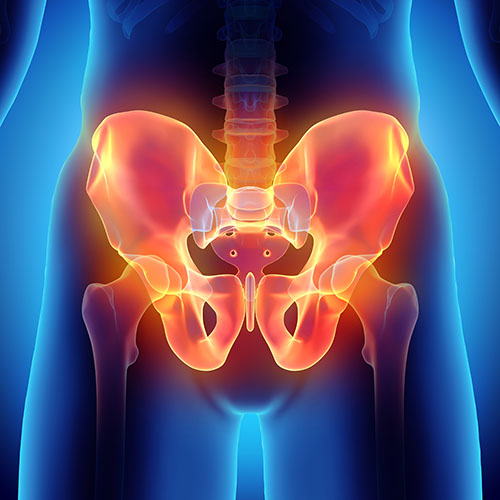
Understanding the Causes of Lower Back and Pelvic Pain
Lower back pain is widespread and has several potential causes, including herniated discs, sprains and strains, poor posture, and spinal arthritis–not to mention various contributing factors like poor posture or muscular weakness.
But if that pain spreads into your pelvic area, there may be something else going on. In fact, lower back pain without a clear underlying cause often stems from dysfunction in the pelvic area, such as the following:
Impaired Pelvic Floor
Did you know that your pelvic floor muscles make up part of your core, which supports and stabilizes your spine? If your pelvic floor muscles are weakened or impaired, your back muscles have to do more work to compensate – setting you up for muscle strains or other injuries.
Sacroiliac Joint Dysfunction
The sacroiliac joint is the joint that links the spine to the pelvis, so it should be surprising that if something’s wrong there, you may feel pain in both your lower back and your pelvic area. Arthritis, injury, and pregnancy can all cause issues in the sacroiliac joint.
Pregnancy
Pregnancy itself is a common cause of pain throughout the lower back and pelvic area. There are two main reasons for this:
- Hormonal changes cause your ligaments to become looser in preparation for childbirth, which puts strain on your lower back and pelvis.
- Your center of gravity changes, and your growing baby can force your hips back at an awkward angle, leading to pain.
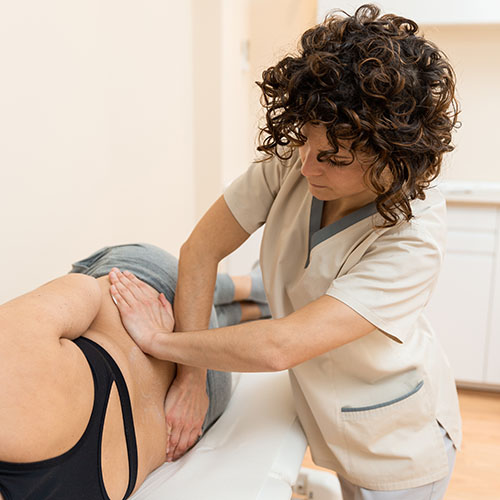
Helping You Find Relief, No Matter the Source
When it comes to pain in your lower back and pelvis, the first step our therapists take is to identify the source of your pain. That way, we can provide the customized treatment you need to resolve the pain at its root rather than merely treating symptoms.
We’ll begin with a comprehensive evaluation. Our therapists provide a welcoming, discreet space where you can freely share your symptoms – including pelvic-related symptoms that might feel embarrassing. Make sure you share…
- The exact location of your pain
- The pain’s sensations–is it burning? Dull? Aching?
- When do you feel pain? Is it persistent? Do you mostly notice it when you wake up?
- Any restrictions in range of motion you might be experiencing
- Any pelvic-related symptoms you might be experiencing, such as incontinence or sexual dysfunction
Once we’ve reviewed your symptoms and taken a full health history, we’ll conduct an in-depth physical evaluation, including running several movement screens. All this information helps us determine whether or not your pain is rooted in your lower back, pelvic area, or somewhere else – and that helps us develop your personalized treatment plan.
Targeted Treatments So You Can Find Relief
Our treatment plans will vary based on your exact needs. In general, though, we aim to help you with the following:
- Find immediate pain relief through manual therapy techniques or gentle stretches
- Improve mobility through targeted range of motion exercises
- Strengthen any weakened or impaired muscles, whether in your back or pelvic floor
- Provide you with the tools you need to avoid future bouts of pain
Call Us Today To Get Started!
If you’re struggling with back or pelvic pain, the Therapy Fit therapists will help you get to the bottom of things. Call to make your appointment today!
Our Patients Get Great Results
“I worked for around month and a half for my low back pain and I saw improvements in few sessions. Right from the start they were excellent. They did an extensive evaluation process which I never expected. They gave me so much information during the evaluation and explained in detail what type of therapy and why I needed them. Their treatment approach is also very good and most importantly they showed so much care and compassion. I will definitely visit this place again in the future if there is a need for physical therapy.”
– Veksha G.

A Quick Introduction to Pelvic Floor Physical Therapy
When was the last time you thought about your pelvic floor? This sling of muscles isn’t visible, but it plays a significant role in our overall health and well-being:
It makes up part of our core muscles, which help us move better and more effectively.
It supports our pelvic organs – bowels, bladder, and, in women, genitals.
If it’s impaired, you can suffer a range of symptoms, from pain to sexual dysfunction.
Pelvic floor physical therapy is a specialized form of physical therapy that focuses on matters of the pelvic floor. It uses the same principles as standard physical therapy, including identifying the source of your discomfort and providing you with a personalized treatment plan.
What Can I Expect From Pelvic Floor Physical Therapy?
• Help with pelvic-related conditions such as incontinence, pelvic pain, sexual dysfunction, or pelvic prolapse.
• A discreet space where you can freely share symptoms and work with a therapist specially trained in women’s health and/or pelvic floor issues.
• Guidance in identifying the deep muscles that might be causing you issues – such as your pelvic floor, deep abdominals, or diaphragm. These muscles are not visible, so working on them can be a challenge.
• Information about using these muscles correctly and targeted exercises to stretch and strengthen them.
• Simple pelvic floor exercise plans that you can do at home.
We offer pelvic floor physical therapy here at Therapy Fit. If you’d like to learn more about what it can do for you, call us today!
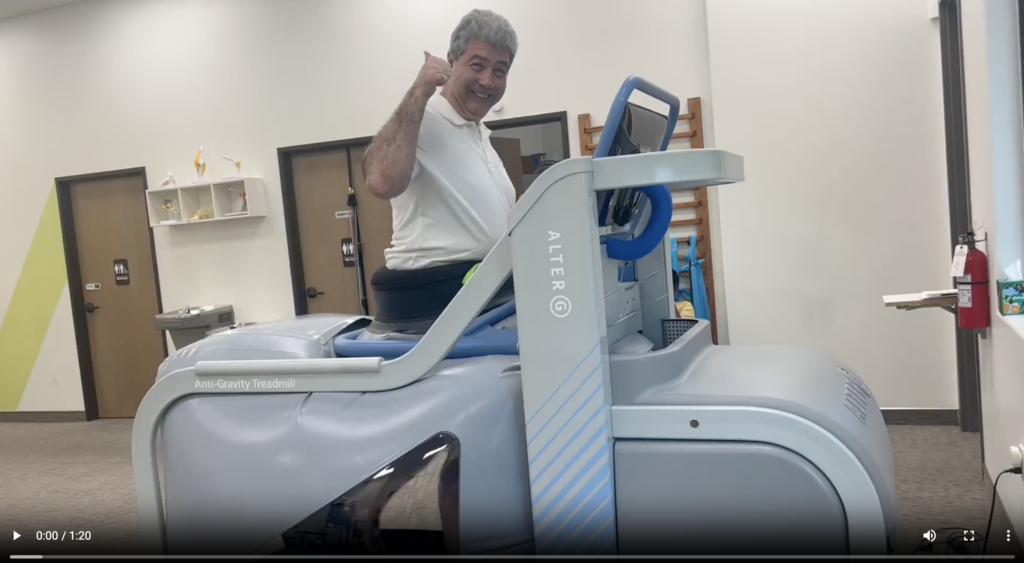
The Alter G Treadmill at Therapy Fit
The term “anti-gravity” admittedly makes it sound like a contraption from a science-fiction universe. In reality, this treadmill was created using advanced contemporary science and technology. The Differential Air Pressure (DAP) technology has been patented by NASA, allowing for a precise calibration of air pressure. The pressurized mechanics of the treadmill act to “unweight” the patient while the machine is in use. By doing so, the patient is able to use the treadmill by seemingly “floating” above it – allowing them to complete their exercise treatments without the harsh foot-to-treadmill impact you get with normal gravity.
Post-operative patients are the prime candidates for the AlterG Treadmill. Patients are strapped into the middle of it, with their feet enclosed in the pressurized case. By safely securing patients, they are able to use the weight-bearing treadmill freely, without pressure on their legs or the fear of falling off of it. Other conditions that have shown improvement through the AlterG Treadmill include tendinitis, obesity, arthritis, Pelvic floor dysfunctions, osteoporosis, plantar fasciitis, shin splints, spine fusions, stress fractures, neurological disorders, complex regional pain syndrome (CRPS), reflex sympathetic dystrophy (RSD), and total joint replacement.


Exercise of the Month
Double Knee To Chest
Start on your back with your knees bent. Slowly bring both knees to your chest. Grasp your knees. Hold for 30 seconds and repeat.




Feel Better by Eating Better!
Anti-Inflammatory Ginger & Turmeric Carrot Soup
This delicious ginger and turmeric carrot soup is as comforting as it is healing. Packed with strong flavors like garlic, fennel, and ginger, and full of anti-inflammatory ingredients, this is the perfect winter soup.
Directions: Heat the olive oil in a large dutch oven or saucepan. Add the fennel, leeks, carrots, and squash. Sauté for 3-5 minutes until the veggies start to soften. Add the garlic, ginger, turmeric, salt, and pepper, and sauté for a few more minutes. Add the broth and coconut milk. Bring the mixture to a boil, cover, and simmer for 20 minutes. Once the soup is cooked, add it to a blender and blend until creamy. You could also use an immersion blender. Taste and adjust the seasonings to your taste. Serve immediately with a dollop of coconut yogurt and enjoy!
https://www.simplyquinoa.com/anti-inflammatory-ginger-turmeric-carrot-soup
Ingredients
- 1 tablespoon olive oil
- 1 leek, cleaned and sliced
- 1 cup chopped fennel bulb (1 small head)
- 3 cups chopped carrots
- 1 cup chopped butternut squash (or more carrots)
- 2 garlic cloves, minced
- 1 tablespoon grated ginger (about a 2-inch piece)
- 1 tablespoon turmeric powder
- Salt & pepper to taste
- 3 cups low-sodium vegetable broth
- 1 can lite coconut milk (14.5 ounces)

Exciting News:
Therapy Fit Expands to Prosper, TX!
We are thrilled to announce the opening of Therapy Fit’s new clinic location in Prosper, TX! Conveniently located at 1630 West Prosper Trail, Suite 510, our new clinic offers the same exceptional care and services you’ve come to expect.
We are now accepting appointments! Call us at (945) 256-1199 or fax us at (972) 535-5940. Our hours are Monday through Friday, 8:00 a.m. to 7:00 p.m., and Saturdays, 9:00 a.m. to 2:00 p.m. We can’t wait to welcome you to our new space and continue supporting your health journey!
Let’s Get You Better ASAP!
Don’t let pain dictate your life. Take the first step towards reclaiming your mobility and well-being with our expert support. Start your journey to a healthier you today.






